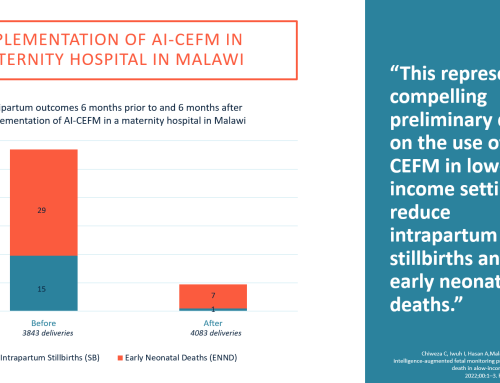
Although it may seem counterintuitive, telemedicine can act as a bridge between vulnerable pregnant people and their providers.
Healthcare IT News: By Kat Jercich November 09, 2020 10:50 AM
This past week, the U.S. Centers for Disease Control and Prevention released a trove of data suggesting that pregnant patients might be at increased risk for severe illness associated with COVID-19.
In light of the statistics, CDC advised that measures to prevent coronavirus infection should be emphasized for pregnant people and their families. Telehealth and virtual care, with its natural distancing, could be one such measure.
Although it may seem counterintuitive, given the hands-on approach obstetricians and gynecologists often take with care, telemedicine can act as a bridge between vulnerable pregnant people and their providers without requiring as much in-person exposure.
Matthew Sappern, CEO and president of PeriGen, told Healthcare IT News that the nature of labor and delivery has created “unique challenges” for clinicians.
“Babies don’t defer coming,” said Sappern in a HIMSS TV interview earlier this year. “I think that made life really difficult for clinicians at these health systems.”
When it comes to staff and patient safety, Sappern told Healthcare IT News this week that remote telemonitoring can be used at facilities as a kind of hub-and-spoke model, with clinicians at a central monitoring station able to track patient health and safety.
“There’s a couple of ways that I’ve seen our solution be helpful in this pandemic,” Sappern said. “In the initial surge we had a bunch of nurses who were really experienced … who couldn’t go to the bedside because they had preexisting conditions or were caregivers,” he continued.
Rather than furlough the nurses – and thus lose out on the clinical expertise they could provide – Sappern said some clients installed them at the central monitoring station. That way, they could be separate from patients while providing guidance to personnel who were not as vulnerable.
Sappern said this style of telemonitoring could allow for separation between COVID-possible or -exposed patients, or those at higher risks for reasons apart from pregnancy. He noted that in rural areas, nurses can provide guidance to other facilities without needing to travel – again reducing potential COVID-19 spread.
PeriGen’s clinical-decision support tools can also help alert providers more quickly to the potential for bad outcomes – which is helpful in an environment with fewer personnel available.
“Technologies like this – that give incremental insight – not only are helping to provide or identify opportunities for intervention in good times, but when you have so much at stake, just by being next to the bedside, these technologies are really helpful,” said Sappern.
The recently released CDC statistics showed that after adjusting for race, age and underlying medical conditions, pregnant people were significantly more likely than nonpregnant people to be admitted to an intensive care unit, to receive invasive ventilation, to receive extra corporeal membrane oxygenation or to die.
The increased risk was particularly notable among Asian people and Native Hawaiian and Pacific Islander people, said the CDC. Given the potential for remote patient monitoring, Sappern said that next steps might include U.S. Food and Drug Administration approval for at-home tools such as fetal heart rate recordings.
“We want to move more into the ambulatory space,” said Sappern.
That’s the avenue doctors at Israel’s Sheba Medical Center are moving toward with their Women’s Health Innovation Center.
As part of the ARC Innovation Center, clinicians at the WHIC are working to launch pilots that concentrate the majority of pregnancy care at home. By inviting multiple vendors to present options for applying their technology to the treatment of pregnant patients, WHIC aims to provide as much assessment for patients and their fetuses as possible without requiring them to physically enter the hospital.
WHIC director Dr. Avi Tsur, an OB-GYN and high-risk pregnancy expert, told Healthcare IT News that gestational diabetes presents an excellent use case for at-home monitoring.
Usually, patients with gestational diabetes “have to come to the clinic quite often,” said Tsur, for a fetal ultrasound and fetal monitoring.
Through the pilot launching next month, said Tsur, “instead of coming to the clinic, they can stay at home and do an online visit.”
The at-home visit requires a patient to use a blood pressure cuff and fetal monitors, both of which connect to a clinical platform. The patient also takes a photo of a urinalysis stick for clinicians to interpret and sweeps an ultrasound on their own stomach. Usually, said Tsur, “they don’t need to be sonographers, there’s no technical challenge.”
“And that’s it!” said Tsur. In doing so, “We replaced a four-hour visit with a half-hour visit with no risk of COVID-19 infection.”
Of course, if the need arises, the WHIC team will ask a patient to come for an in-person appointment. Telehealth is, as many advocates have said, complementary to in-office treatment, not a full replacement for it.
Still, Tsur stressed, remote care and telemedicine are things that are technical possibilities.
“Only a few good things came from the COVID-19 spread, and one of them is definitely remote care,” he said via a statement. “Now that we know we can treat many of our patients at home, we will never return to wasting their time and bringing them to the hospital where they may be infected.”